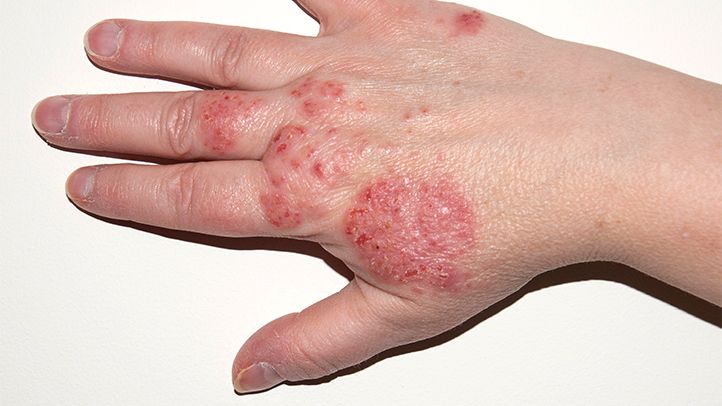
- Between 15% and 20% of children worldwide have an inflammatory skin condition known as eczema.
- Results from a phase 3 clinical trial found the medication dupilumab provides at least a 75% improvement in eczema symptoms in children ages 6 months to 5 years old.
- U.S. regulators approved the use of dupilumab in children ages 6 months to 5 years of age in June 2022.
Between 15% and 20% of children around the world have eczema — an inflammatory skin condition that is currently incurable.
Because of its symptoms, past research shows children with eczema — clinically known as atopic dermatitisTrusted Source — face higher rates of mental healthTrusted Source issues such as depressionTrusted Source and anxiety. They may also struggle with sleepingTrusted Source.
Now, a phase 3 clinical trial recently publishedTrusted Source in The Lancet reports that the drug dupilumabTrusted Source provided at least a 75% improvement in eczema symptoms by week 16 in children ages 6 months to 5 years old when used in conjunction with a topical corticosteroid
What is eczema?
Atopic dermatitis is a chronic inflammatory skin disease caused by a variety of reasons, including a person’s inflammatory response, certain triggers, genetic history, and stress.
Symptoms of eczema include:
- extremely dry, flakey, and/or cracked skin
- rashes on the neck, wrists, and ankles, or behind the elbows and knees, in children
- itching
- red, irritated skin
- blisters/sores that easily break and leak fluid
There is currently no cure for atopic dermatitis, but doctors treat flare-ups of the disease as well as provide preventative measures for future outbreaks.
Traditional eczema symptom medications include:
Atopic dermatitis in children
Eczema is common in children. Research shows that 60% of childrenTrusted Source first develop eczema symptoms during the first year of life, with some children outgrowing eczemaTrusted Source as they near adulthood.
“Babies and young children with uncontrolled atopic dermatitis may be constantly scratching, irritable, and awake multiple times in the night with their parents, which can impact (the) quality of life for both the children and their parents,” explained Dr. Amy S. Paller, the chair of dermatology and professor of pediatrics at Northwestern University Feinberg School of Medicine in Illinois and a principal investigator of the phase 3 clinical trial.
According to Paller, there was a need for treatment options for infants and young children with uncontrolled moderate-to-severe atopic dermatitis before the Food and Drug Administration approved the use of Dupixent in children ages 6 months to 5 years of age with moderate-to-severe atopic dermatitis in June 2022.
“The treatment options for patients between the ages of 6 months and 5 years were mostly limited to topical steroids,” she explained to Medical News Today. “Given that the options otherwise were only immune suppressants like oral steroids, cyclosporine, and methotrexate, we as pediatric dermatologists were very hesitant to move to anything beyond topical steroids. And, frankly, even worried about using potent steroids chronically, which some of these children with moderate-to-severe eczema need for even partial control.”
What is dupilumab?
Dupixent (dupilumab) is a medication created by Regeneron Pharmaceuticals Inc. and jointly developed by Regeneron and Sanofi.
The Food & Drug Administration (FDA) first approvedTrusted Source Dupixent for the treatment of atopic dermatitis in adults in March 2017. The FDA then expanded the use of Dupixent in 2020 for children ages 6 to 11 years old before the approval earlier this year for children ages 6 months to 5 years of age.
Paller stated that dupilumab is a biologic medicineTrusted Source that works to help address an underlying source of inflammation — called type 2 inflammationTrusted Source — that contributes to atopic dermatitis. She added that dupilumab is not an immunosuppressantTrusted Source or steroidTrusted Source.
“Many parents and caregivers of babies and young children with uncontrolled moderate-to-severe atopic dermatitis have tried multiple topical therapies, and some have even tried systemic steroids or broad immunosuppressants, and still remain uncontrolled, which leaves them searching for new options,” she explained. “Long-term use of corticosteroids and off-label immunosuppressants can be temporarily effective but can also be associated with significant side effects.”
Dupilumab efficacy for young children
The phase 3 clinical trial evaluated the safety and efficacy of dupilumab in 162 children ages 6 months and 5 years with uncontrolled moderate-to-severe atopic dermatitis.
The study participants either received an injected dose of the medication every four weeks in conjunction with a low-potency topical corticosteroid, or just the topical corticosteroid in the placebo group.
After 16 weeks of treatment, researchers reported more than half of the participants receiving dupilumab had at least a 75% improvement in their Eczema Area and Severity Index (EASI-75). Medical professionals use the EASI-75 to measure the number of inflamed areas on the body and their severity.
Researchers also found that 48% of participants receiving dupilumab had a reduction in itchiness and 28% had almost-clear or clear skin after 16 weeks.
“The research showed the effect of dupilumab for most of these younger children is dramatic and at least as good as we’ve seen with the riskier immunosuppressant medications,” Paller commented. “Importantly, although the dupilumab is an every 4-week injection, there just is a huge safety advantage and the children do not need the frequent blood draws to monitor the safety required for other medications — in fact, no blood draws are needed with dupilumab.”
Evaluating safety
In regards to safety, the research team reported a safety profile similar to that of patients 6 years and older taking dupilumab for atopic dermatitis.
The most common adverse effects observed in the children participating in the dupilumab group during the clinical trial included:
- herpes viral infection (6%)
- pink eye, clinically known as conjunctivitis (5%)
- molluscum contagiosum (5%)
- runny nose, clinically known as rhinorrhea (5%)
- tooth decay or dental cavities, clinically known as dental caries (5%)
“Dupilumab has been studied in a number of extensive clinical trial programs and has demonstrated a strong safety profile across a number of age groups, and has been studied up to one year in young children,” Paller reported. “Safety results from the trial, as well as a one-year open-label extension trial, in children aged 6 months to 5 years were generally consistent with the known safety profile of dupilumab in patients 6 years and up. That is limited to some reactions at the site of injection, which actually were not seen compared to placebo in the trials in these 6-month to 5-year-old children, and some increased eye redness or conjunctivitis — still in the minority and managed with some medication.”
‘Super exciting data’
MNT also spoke with Dr. Emma Guttman-Yassky, a professor and system chair for The Kimberly and Eric J. Waldman Department of Dermatology at the Icahn School of Medicine at Mount Sinai in New York, about this clinical trial data.
“This is super exciting data, as until now we did not have safe and effective treatments for our atopic dermatitis patients,” she said. “Dupilumab is a specific immune modulator that is safe for long-term use, unlike previously used immune suppressants that are not so safe for long-term use.”
When asked about the safety profile of dupilumab, Guttman-Yassky commented, “it’s important to tell parents about the possibility of conjunctivitis/dry eye condition, but overall the safety profile was very good.”
Guttman-Yassky also mentioned there is some additional research she would like to see for dupilumab.
“I would like to see minimally invasive biomarker approaches, such as tape stripsTrusted Source, that we have shown in infants and children utilized in such studies to inform on pathogenesis,” she said.
- Eczema or atopic dermatitis is an inflammatory skin disease affecting about 3% of adults and 20% of children around the world.
- Past research shows certain foods, such as cow’s milk dairy, can trigger eczema symptoms.
- Researchers from McMaster University found eliminating potentially problematic foods may not be enough to alleviate disease symptoms.
Atopic dermatitis — also known as eczema — affects up to 3% of adults and 20% of children globally.
Different allergens and irritants in the environment can trigger the body’s immune system, causing eczema flares. These triggers can include environmental pollutants, pollen, fragrances, and even stress.
Past research also shows certain foods can trigger eczema symptoms, particularly in people with a particular gene variant. These foods include wheat, nutsTrusted Source, eggsTrusted Source, and dairy.
Now, scientists from McMaster University in Canada have added to the collective research regarding eczema and food triggers. They report that people with mild to moderate eczema may reduce symptoms when eliminating certain foods, including dairy products.
However, they note just making dietary changes alone may not be enough — people may still need to continue medical treatments as well.
Eczema and food allergies
According to Dr. Derek Chu, an assistant professor of medicine at McMaster University and lead author of the new study, the influence of diet on atopic dermatitis is complex and the use of dietary elimination as a treatment has historically conflicting views.
“Patients and caregivers commonly report strong suspicion and historical teaching among clinicians provided a greater emphasis on the role of food allergy as a driver of atopic dermatitis,” he explained to Medical News Today (MNT). “However, many clinicians now cast doubt and consternation out of concern for confounding from other triggers or atopic dermatitis flare independent of external factors and avoiding harms that can occur with dieting practices.”
“As a result, some patients found current approaches to discussing dietary concerns with their care providers unhelpful, which in turn led to frequent unsupervised and potentially harmful dietary eliminations,” he added.
For example, Chu stated people may suspect any kind of food as contributing to their atopic dermatitis. One food associated in the past as a potential trigger for eczema is dairy products made from cow’s milkTrusted Source.
“Milk is among the most commonly suspected allergens in infants and children,” he explained. “Dairy, in general, is a common food across all ages, both of which likely contribute to patients and caregivers associating it with flares of atopic dermatitis.”
A study in 2002 found children who drank cow’s milk increased their risk of developing additional food allergies and persistent atopic dermatitis.
However, other research shows lower levels of vitamin D — which is found in cow’s milk products — may lead to increased atopic dermatitis symptoms.


I need a job
Sent from my iPhone
>
LikeLike